Diagnosis of paediatric tuberculosis. Application of metabonomics to identify host biomarkers in serum
Diagnosis of tuberculosis (TB) in children remains challenging and developing better diagnostics is a priority. Diagnostic tools that perform well in adults fail to diagnose two-thirds of children with suspected TB due to the paucibacillary nature of paediatric disease. Age, as well as the development of the immune system, further complicates assessment, as the performance of tests for latent TB infection varies with age. The non-specific clinical presentation of TB in children presents a further diagnostic challenge. In developing countries, where the majority of the burden of TB disease lies, approximately 40% of patients are incorrectly diagnosed. Consequently, many children are not appropriately treated, and over 210,000 children are estimated to die every year.
Can metabolic profiling of sera distinguish children with TB from children with other diseases?
In this case-control study, 112 symptomatic children under the age of 15 years old with presumptive TB were recruited in The Gambia and classified as bacteriologically-confirmed TB, clinically diagnosed TB, or as other diseases. A validation cohort of 36 children from the UK with TB were also recruited.
Sera were analysed using untargeted 1H nuclear magnetic resonance (NMR) spectroscopy and three ultra-performance liquid chromatography-mass spectrometry (UPLC-MS) assays to maximise coverage of the sera metabolome (measuring polar metabolites and complex lipid species). Multivariate data analysis was used to distinguish patients with TB from other diseases and the diagnostic accuracy of the identified discriminating metabolites was evaluated by producing Receiver Operating Characteristic (ROC) curves.
Systematic differences between cases and controls included increased concentrations of glutamate, acetylated glycoproteins and phenylalanine in the TB disease sera, as well as a number of lipids, mostly ceramaides. These panels of discriminatory metabolites yielded a diagnostic performance for paediatric TB comparable to that of Xpert MTB/RIF and interferon gamma release assays.
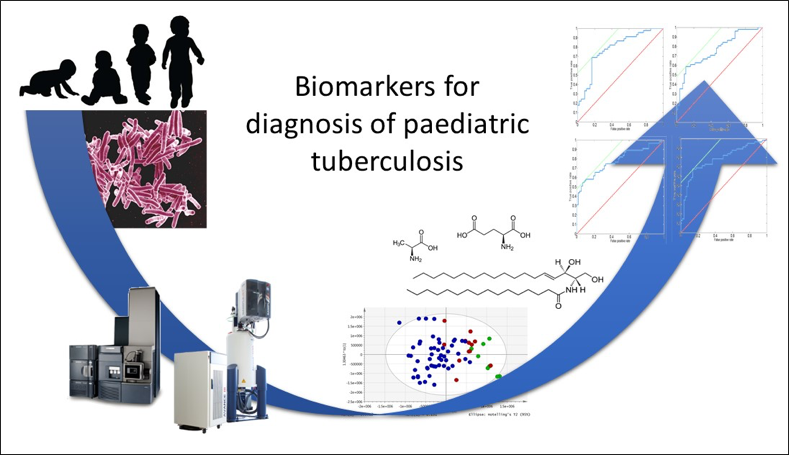
The NPC have demonstrated that alterations in host metabolism in paediatric TB are detectable using metabonomic techniques applied to serum samples. The metabolic profiles provided insights into the pathological processes associated with TB, but further validation is required to assess the clinical utility of this diagnostic approach in the context of screening algorithms.
Further work will include integration of datasets as this may provide better predictive ability than each technique alone, development of a UPLC-MS targeted method including the most predictive metabolites and validation in an independent patient cohort. A parallel study will investigate if urinary metabolites can also distinguish children with TB from children with other diseases.
Metabolome to Product
A suitable point-of-care test based on quantitative analysis of metabolites for the rapid and accurate diagnosis of tuberculosis in children
Acknowledgements: Infrastructure support was provided by the National Institute for Health Research (NIHR) Imperial Biomedical Research Centre (BRC)
Return to Case Studies